Introduction
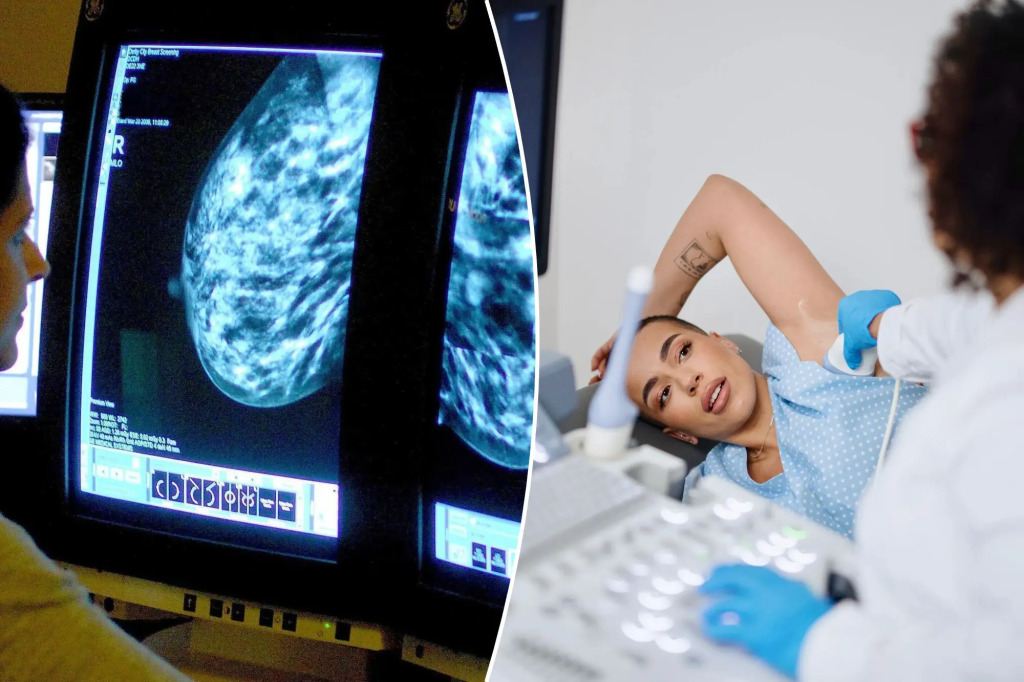
Women’s cancer screening plays a critical role in early detection, timely treatment, and improved survival rates. Screenings such as mammograms, Pap smears, HPV testing, and colorectal exams can identify cancer at its earliest and most treatable stages. Despite strong clinical evidence supporting these preventive measures, screening rates among women remain lower than recommended across many populations.
At First Point MD, preventive care is a cornerstone of long-term health. Understanding the barriers that prevent women from accessing cancer screening—and implementing effective strategies to overcome them—is essential to improving health outcomes, reducing disparities, and empowering women to take control of their health.
Why Women’s Cancer Screening Is Essential
Cancer remains one of the leading causes of death among women worldwide. However, many cancers are highly treatable when detected early.
Common Screenings for Women
Breast cancer: Mammography
Cervical cancer: Pap smear and HPV testing
Colorectal cancer: Colonoscopy or stool-based tests
Ovarian and uterine cancer: Risk-based evaluation and symptom assessment
Regular screening can significantly reduce mortality by enabling early diagnosis and less aggressive treatment options.
Key Barriers to Women’s Cancer Screening
Multiple factors—social, economic, cultural, and systemic—contribute to low screening uptake among women. These barriers often overlap, compounding their impact.
Lack of Awareness and Health Education
One of the most common barriers is limited awareness about cancer risks and screening guidelines.
Contributing Factors
Misunderstanding of screening intervals
Lack of knowledge about symptoms
Confusion between screening and diagnostic tests
Belief that screening is unnecessary without symptoms
Many women mistakenly assume that feeling healthy means screening is not needed, delaying detection until symptoms appear.
Fear, Anxiety, and Emotional Barriers
Emotional responses strongly influence healthcare decisions.
Common Fears Include
Fear of a cancer diagnosis
Anxiety about test results
Concern about pain or discomfort during procedures
Worry about invasive examinations
For some women, the emotional burden of screening feels heavier than the perceived benefit, especially without proper counseling and reassurance.
Cultural and Social Influences
Cultural beliefs and social norms can significantly affect women’s participation in cancer screening programs.
Examples of Cultural Barriers
Stigma surrounding cancer discussions
Modesty concerns related to physical exams
Gender preferences for healthcare providers
Mistrust of the healthcare system
In certain communities, women may prioritize family responsibilities over their own health, postponing preventive care.
Financial and Insurance Challenges
Cost remains a major obstacle for many women.
Financial Barriers Include
Lack of health insurance
High out-of-pocket costs
Limited coverage for preventive services
Lost wages due to time off work
Even when screenings are covered, uncertainty about costs can discourage women from scheduling appointments.
Limited Access to Healthcare Services
Access issues disproportionately affect women in rural or underserved areas.
Access-Related Challenges
Long travel distances to screening centers
Limited clinic hours
Shortage of female healthcare providers
Transportation difficulties
These logistical challenges often result in missed or delayed screenings.
Time Constraints and Competing Responsibilities
Women frequently juggle multiple roles, including caregiving, work, and household responsibilities.
Impact on Screening
Difficulty scheduling appointments
Inability to take time off work
Prioritizing family needs over personal health
Preventive care is often postponed when immediate responsibilities take precedence.
Healthcare System Barriers
System-level factors can also reduce screening uptake.
Common Systemic Issues
Inadequate provider recommendations
Poor follow-up reminders
Fragmented care coordination
Limited patient-provider communication
Women are significantly more likely to undergo screening when their healthcare provider actively recommends it.
Strategies to Improve Women’s Cancer Screening Uptake
Addressing barriers requires a comprehensive, patient-centered approach that combines education, accessibility, and trust.
Enhancing Patient Education and Awareness
Clear, culturally sensitive education is foundational.
Effective Education Strategies
Community outreach programs
Educational materials in multiple languages
Clear explanations of screening benefits and guidelines
One-on-one counseling during routine visits
At First Point MD, patient education is integrated into every preventive care interaction.
Improving Provider Communication and Trust
Strong patient-provider relationships increase screening participation.
Key Approaches
Active listening and empathy
Clear explanation of procedures
Addressing fears and misconceptions
Encouraging shared decision-making
When women feel respected and informed, they are more likely to engage in preventive care.
Reducing Financial Barriers
Cost-related obstacles can be minimized through coordinated efforts.
Solutions Include
Insurance navigation assistance
Transparent pricing information
Referral to low-cost or covered screening programs
Educating patients about preventive care benefits
Proactive financial guidance removes uncertainty and builds confidence.
Expanding Access and Convenience
Making screening more accessible increases participation.
Access-Focused Strategies
Extended clinic hours
Telehealth pre-screening consultations
Mobile screening units
Streamlined scheduling systems
Convenience plays a significant role in preventive health behaviors.
Leveraging Technology and Reminder Systems
Digital tools can significantly improve screening adherence.
Examples
Automated appointment reminders
Patient portals for test scheduling
Educational email or text campaigns
Electronic health record alerts
These tools help women stay on track with recommended screenings.
Culturally Competent and Inclusive Care
Cultural sensitivity is essential for equitable healthcare.
Best Practices
Diverse healthcare teams
Gender-concordant provider options
Respect for cultural beliefs
Community-based partnerships
Culturally competent care fosters trust and improves long-term engagement.
The Role of Preventive Care at First Point MD
At First Point MD, women’s preventive health is a priority.
Our Commitment Includes
Personalized screening recommendations
Comprehensive preventive evaluations
Patient-centered communication
Ongoing follow-up and support
By addressing both medical and non-medical barriers, First Point MD helps women take proactive steps toward early cancer detection.
Long-Term Benefits of Improved Screening Uptake
Increasing women’s cancer screening participation leads to:
Earlier diagnosis
Less aggressive treatment
Lower healthcare costs
Improved survival rates
Enhanced quality of life
Preventive care strengthens not only individual health but also community well-being.
Conclusion
Barriers to women’s cancer screening are complex and multifaceted, ranging from emotional and cultural concerns to financial and systemic challenges. However, these obstacles are not insurmountable.
Through education, improved access, compassionate care, and patient-centered strategies, healthcare providers can significantly increase screening uptake. At First Point MD, we are committed to empowering women with the knowledge, resources, and support they need to prioritize preventive care.
Early detection saves lives—and removing barriers to screening is one of the most effective ways to protect women’s health today and for the future.